The Importance of Elderly Care for Grandparents
Ensuring proper elderly care for grandparents is of paramount importance. As grandparents age, their needs change, and it becomes crucial to provide them with the necessary support and assistance to maintain their well-being. Understanding the changing needs of grandparents and investing in elderly care can significantly enhance their quality of life.

Understanding the Changing Needs of Grandparents
Grandparents play a vital role in families, and as they age, their physical and mental health may deteriorate. They may face challenges such as chronic health conditions, limited mobility, memory loss, and the need for assistance with daily activities. Recognizing these changing needs is crucial to ensure that appropriate care is provided.
It’s essential to assess the specific requirements of grandparents in terms of health, mobility, and emotional well-being. This evaluation helps determine the level of care needed and the type of elderly care option that best suits their unique situation.
The Benefits of Investing in Elderly Care
Investing in elderly care for grandparents offers numerous benefits that contribute to their overall well-being and happiness. Some key advantages include:
- Professional Assistance: Elderly care services provide access to trained professionals who specialize in senior care. These professionals have the expertise to handle the physical and emotional needs of grandparents effectively.
- Enhanced Safety and Security: Elderly care facilities and in-home care services ensure a safe and secure environment for grandparents. They incorporate safety measures, such as fall prevention strategies and emergency response systems, to minimize potential risks.
- Social Interaction: Loneliness and social isolation can negatively impact the mental health of seniors. Elderly care options offer opportunities for social interaction and engagement with peers, helping to combat feelings of loneliness and promoting overall well-being.
- Specialized Care: Different elderly care options cater to specific needs. Whether it’s in-home care, assisted living facilities, or nursing homes, each option provides specialized care tailored to the requirements of grandparents. This ensures that they receive the appropriate level of support and assistance.
- Peace of Mind: Investing in elderly care for grandparents provides peace of mind to both the grandparents and their families. Knowing that their loved ones are receiving the care they need, families can focus on their own responsibilities while ensuring the well-being of their grandparents.
By understanding the changing needs of grandparents and recognizing the benefits of investing in elderly care, families can make informed decisions to provide the best possible care for their beloved grandparents. Whether it’s in-home care, assisted living facilities, or nursing homes, each option offers unique advantages that contribute to the overall quality of life for grandparents in their golden years.
Types of Elderly Care Options
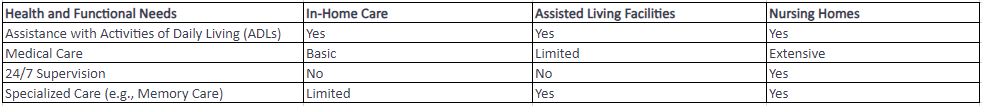
When it comes to providing care for grandparents, there are several types of elderly care options available. Each option caters to different needs and preferences, ensuring that your grandparents receive the appropriate level of care and support. The three main types of elderly care options are in-home care, assisted living facilities, and nursing homes.
In-Home Care
In-home care allows your grandparents to receive care in the comfort of their own home. This option is ideal for individuals who prefer to age in familiar surroundings and maintain independence. In-home care services can be tailored to meet specific needs, ranging from basic assistance with daily activities to more comprehensive medical care.
In-Home Care Services
- Personal care assistance (bathing, grooming)
- Medication management
- Meal preparation
- Light housekeeping
- Companionship and emotional support
In-home care is often provided by professional caregivers who visit your grandparents’ home on a scheduled basis. They can help with tasks such as personal care, medication management, meal preparation, light housekeeping, and provide companionship. This option allows grandparents to maintain their daily routines while receiving the necessary support.
Assisted Living Facilities
Assisted living facilities are residential communities designed for seniors who require assistance with daily activities but do not need extensive medical care. These facilities offer a combination of housing, personal care services, and social activities to promote a comfortable and engaging lifestyle.
Assisted Living Facilities
- Private or semi-private living spaces
- Assistance with activities of daily living (ADLs)
- Social and recreational activities
- On-site dining services
- Transportation services
Assisted living facilities provide private or semi-private living spaces, allowing your grandparents to have their own personal space while still having access to care and support. Trained staff members are available to assist with activities of daily living (ADLs), such as bathing, dressing, and medication management. Additionally, these facilities offer social and recreational activities, on-site dining services, and transportation services to enhance the quality of life for residents.
Nursing Homes
Nursing homes, also known as skilled nursing facilities, provide comprehensive care for seniors who have complex medical needs or require around-the-clock assistance. This option is suitable for grandparents who need specialized medical care and monitoring due to chronic conditions or disabilities.
Nursing Home Services
- 24/7 skilled nursing care
- Rehabilitation services
- Medication management
- Social activities and programs
- Dietary and nutrition services
Nursing homes offer 24/7 skilled nursing care, ensuring that your grandparents’ medical needs are attended to at all times. These facilities also provide rehabilitation services to help seniors recover from illnesses or injuries. Additionally, nursing homes offer social activities and programs to promote socialization and engagement, as well as dietary and nutrition services to ensure proper nutrition.
When deciding on the best elderly care option for your grandparents, it’s important to consider their specific needs, preferences, and the level of care required. Discussing these options with your grandparents and consulting with healthcare professionals can help you make an informed decision that ensures their well-being and enhances their quality of life.
Factors to Consider When Choosing Elderly Care
When it comes to choosing the right elderly care for your grandparents, there are several factors that need to be carefully considered. By taking these factors into account, you can ensure that the chosen care option aligns with their specific needs and preferences. The key factors to consider include assessing health and functional needs, evaluating financial considerations, and considering personal preferences.
Assessing the Health and Functional Needs
Assessing the health and functional needs of your grandparents is a crucial step in determining the appropriate level of care required. Consider their medical conditions, mobility, and daily living activities. This assessment will help you determine whether they require minimal assistance at home or if they need a higher level of care provided by a facility.
Evaluating Financial Considerations
Evaluating the financial considerations associated with elderly care is essential to ensure that the chosen option fits within the budget. The cost of care can vary significantly based on the type of care, location, and level of assistance required. Consider factors such as income, savings, insurance coverage, and government assistance programs.

Considering Personal Preferences
Considering the personal preferences of your grandparents is crucial to ensure their comfort and happiness in the chosen care option. Take into account their preferences regarding the location, social activities, and level of independence they desire. Involve them in the decision-making process to ensure that their voices are heard and their preferences are respected.

By carefully assessing the health and functional needs, evaluating financial considerations, and considering personal preferences, you can make an informed decision when choosing the right elderly care for your grandparents. Remember to involve them in the process and seek professional guidance if needed to ensure that their care needs are met effectively.
Planning for Elderly Care
When it comes to providing elderly care for grandparents, careful planning is essential to ensure their well-being and meet their specific needs. This section will discuss three key aspects of planning for elderly care: creating a care plan, addressing legal and financial considerations, and effectively communicating with grandparents about care options.
Creating a Care Plan
Creating a comprehensive care plan is the first step in ensuring that your grandparents receive the necessary support and assistance. A care plan outlines the specific care requirements, schedules, and responsibilities, providing a roadmap for caregivers and family members. Consider the following factors when developing a care plan:
- Healthcare needs: Assess the physical and medical needs of your grandparents, including medication management, doctor’s appointments, and any specialized care required.
- Daily activities: Determine the assistance needed with activities of daily living (ADLs) such as bathing, dressing, eating, and mobility.
- Social engagement: Include opportunities for social interaction and engagement to promote mental and emotional well-being.
- Safety measures: Identify and address potential safety concerns, such as fall prevention, home modifications, and emergency preparedness.
Creating a care plan allows you to organize and prioritize the care of your grandparents, ensuring that their needs are met effectively.
Legal and Financial Considerations
When planning for elderly care, it’s important to address the legal and financial aspects to protect your grandparents’ interests. Consider the following key considerations:
- Estate planning: Encourage your grandparents to create or update their wills, establish power of attorney, and determine their healthcare directives.
- Financial management: Assess their financial situation and explore options such as long-term care insurance, Medicare, and Medicaid to determine the best financial resources for their care.
- Legal documents: Ensure that important legal documents, such as advance healthcare directives and durable power of attorney, are in place to guide decision-making in case your grandparents are unable to do so.
Addressing legal and financial considerations provides peace of mind and ensures that your grandparents’ assets and personal affairs are managed properly during their elderly care journey.
Communicating with Grandparents about Care Options
Open and effective communication with your grandparents is crucial when discussing care options. Here are some tips for successful communication:
- Empathy and respect: Approach the conversation with empathy and respect, acknowledging their desires, concerns, and preferences.
- Active listening: Give your grandparents an opportunity to express their thoughts and concerns. Listen attentively to understand their needs and wishes.
- Provide information: Educate your grandparents about the different care options available, explaining the benefits and potential challenges of each choice.
- Involve them in decision-making: Involve your grandparents in the decision-making process, allowing them to have a say in their care and respecting their autonomy.
By fostering open and honest communication, you can ensure that your grandparents feel involved and empowered in the decision-making process, creating a sense of ownership and comfort in their elderly care journey.
Planning for elderly care requires careful consideration of various factors, including creating a care plan, addressing legal and financial aspects, and maintaining effective communication with your grandparents. By taking these steps, you can provide the necessary support and ensure a positive and nurturing environment for your grandparents’ well-being.
Resources and Support for Elderly Care
When it comes to providing the best possible care for grandparents, there are various resources and support options available. These resources can help in navigating the complexities of elderly care and ensure that your grandparents receive the assistance they need. Here are some key avenues to explore:
Local Agencies and Organizations
Local agencies and organizations dedicated to elderly care can be valuable sources of information and support. These entities often provide a range of services, including assistance with healthcare, housing, and social programs. They can help you access resources specific to your location and connect you with professionals who specialize in elderly care.
Type of Resource/Organization and Services Provided
- Area Agency on Aging: Assistance with long-term care options, home-based services, and caregiver support programs
- Senior Centers: Social activities, educational programs, and access to community resources
- Nonprofit Organizations: Support groups, counseling services, and educational workshops
Online Resources and Support Groups
The internet offers a wealth of resources for those seeking information and support in elderly care. Online platforms provide a convenient way to access a wide range of articles, guides, and forums where you can connect with others facing similar challenges. Online support groups can provide a sense of community, allowing you to share experiences and learn from others.
Type of Online Resource and Services Provided
- Government Websites: Information on Medicare, Medicaid, and other public programs
- Health Websites: Articles, blogs, and forums on elderly care topics
- Social Media Groups: Online communities for sharing experiences, advice, and support
Professional Guidance and Advice
Seeking professional guidance and advice is crucial when making decisions regarding elderly care. Experts in the field can provide personalized recommendations based on your grandparents’ specific needs and circumstances. Professionals who can offer valuable insights include geriatric care managers, elder law attorneys, financial advisors, and healthcare providers specialized in geriatrics.
Type of Professional and Services Provided
- Geriatric Care Managers: Comprehensive assessment, care planning, and coordination of services
- Elder Law Attorneys: Legal advice on estate planning, long-term care planning, and guardianship
- Financial Advisors: Assistance with financial planning, insurance options, and long-term care funding
- Geriatric Healthcare Providers: Medical care, medication management, and specialized treatment plans
By utilizing these resources and support options, you can ensure that your grandparents receive the care and support they deserve. Remember to tailor your approach based on their unique needs and preferences. Providing elderly care for your grandparents is a journey, and having access to the right resources will make it a smoother and more fulfilling experience.
Sources
A Guide to Taking Care of Grandparents | Eastleigh Care Homes